Over 10 million American adults experience seasonal depression each year, impacting not only mood but also the risk of developing addictions. As the seasons shift, many find themselves battling overwhelming sadness and turning to substances for relief. Understanding how seasonal depression and addiction often overlap gives families and professionals vital insight into early warning signs, potential risks, and better strategies for care. The right information can make all the difference in breaking this cycle.
Table of Contents
- Defining Seasonal Depression and Addiction
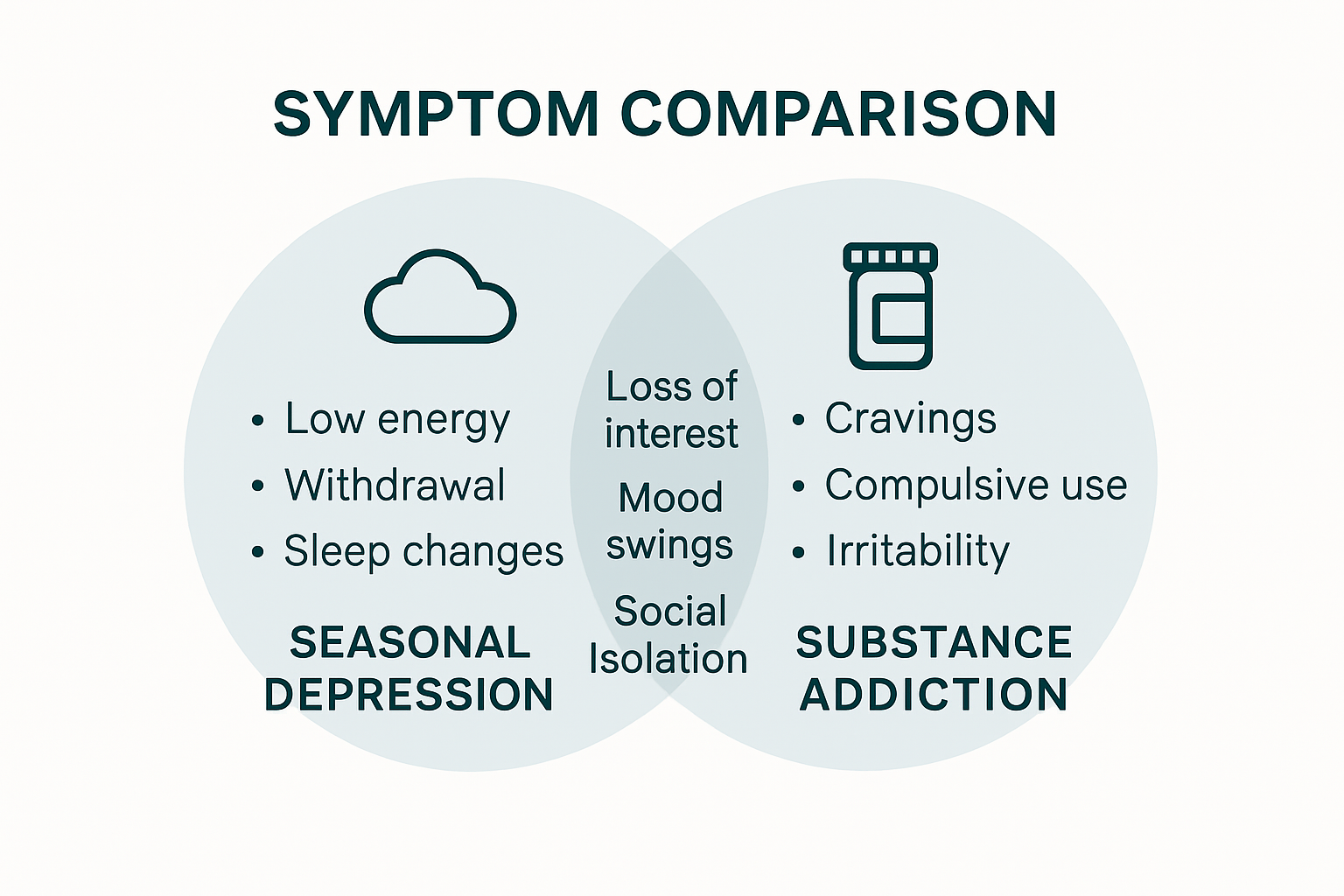
- Recognizing Symptoms and Overlapping Signs
- Why Seasonal Changes Trigger Substance Use
- Risk Factors Unique to Los Angeles Area
- Effective Treatment for Co-Occurring Conditions
- Supporting Loved Ones During Seasonal Changes
Key Takeaways
| Point | Details |
|---|---|
| Understanding SAD | Seasonal Affective Disorder (SAD) is a form of depression linked to seasonal changes, particularly impacting mood during fall and winter months. |
| Connection to Addiction | Individuals with SAD may use substances to cope, leading to a dangerous cycle of self-medication and worsening substance abuse problems. |
| Local Risk Factors | In the Los Angeles area, high-stress environments and cultural pressures can exacerbate the risks associated with seasonal depression and addiction. |
| Integrated Treatment Approaches | Effective recovery requires a comprehensive treatment strategy that addresses both seasonal depression and potential substance abuse simultaneously. |
Defining Seasonal Depression and Addiction
Seasonal Depression and Addiction represent complex psychological challenges that intertwine mental health and substance abuse patterns. Seasonal Affective Disorder (SAD) is a specific type of depression characterized by recurring mood episodes that follow predictable seasonal patterns, typically emerging during specific times of the year.
Understanding SAD requires recognizing its nuanced presentation. Research indicates that these depressive episodes often manifest during late autumn and winter months, with symptoms remitting as seasonal conditions change. The disorder goes beyond typical mood fluctuations, representing a significant mental health condition that can profoundly impact an individual’s emotional stability and behavioral patterns.
The connection between seasonal depression and addiction is particularly critical. Individuals experiencing SAD might turn to substances as a coping mechanism, creating a dangerous cycle of self-medication. Alcohol, drugs, and other addictive behaviors can temporarily alleviate depressive symptoms, but ultimately exacerbate underlying mental health challenges. This psychological dependency can lead to more severe substance use disorders, making integrated treatment approaches essential for comprehensive recovery.
Key characteristics of seasonal depression include:
- Persistent low mood during specific seasons
- Significant changes in energy levels and motivation
- Disrupted sleep patterns
- Increased risk of substance abuse as a coping mechanism
- Potential for developing more complex mental health challenges
Recognizing these patterns is the first step toward effective intervention and healing. Professional support from specialized addiction recovery centers can provide targeted strategies for managing both seasonal depression and potential substance abuse challenges.
Recognizing Symptoms and Overlapping Signs
Seasonal depression represents a complex mental health challenge with symptoms that can significantly disrupt daily functioning. Specific symptoms of Seasonal Affective Disorder (SAD) vary depending on the season, creating unique challenges for individuals experiencing these cyclical mood disorders.
Research highlights that SAD symptoms extend far beyond typical mood fluctuations. Individuals may experience profound psychological and behavioral changes, including:
- Social withdrawal
- Decreased work or academic performance
- Increased vulnerability to substance abuse
- Potential development of concurrent mental health conditions
- Heightened risk of anxiety or eating disorders
The intersection between seasonal depression and addiction creates a particularly dangerous psychological landscape. Individuals often use substances as a temporary mechanism to manage overwhelming emotional challenges. This self-medication approach can rapidly transform into a destructive cycle where substance use becomes a primary coping strategy, ultimately exacerbating both mental health and addiction issues.
Critical warning signs that suggest the potential overlap of seasonal depression and addiction include:
- Persistent mood changes coinciding with specific seasonal patterns
- Increased alcohol or drug consumption during depressive periods
- Significant changes in sleep and energy levels
- Emotional instability and unpredictable behavioral patterns
- Withdrawal from social connections and support systems
Understanding these interconnected symptoms is crucial for developing comprehensive treatment strategies. Professional addiction recovery centers can provide integrated approaches that address both the underlying mental health challenges and potential substance abuse patterns.
Why Seasonal Changes Trigger Substance Use
Seasonal changes create profound psychological challenges that can dramatically increase an individual’s vulnerability to substance abuse. Research demonstrates that Seasonal Affective Disorder (SAD) manifests through cyclical depressive episodes closely tied to specific times of the year, typically fall and winter months, which can significantly impact emotional regulation and coping mechanisms.
Clinical studies reveal that individuals frequently turn to alcohol and other substances as a self-medication strategy to manage uncomfortable emotional states. This desperate attempt to alleviate depressive symptoms creates a dangerous psychological pattern where substance use becomes a primary coping mechanism, potentially leading to more severe addiction challenges.
The neurochemical changes accompanying seasonal shifts play a critical role in triggering substance abuse. Reduced sunlight during winter months can disrupt serotonin and dopamine production, leading to decreased mood stability and increased psychological distress. These neurological alterations make individuals more susceptible to seeking chemical interventions that temporarily mask emotional pain, creating a complex cycle of dependency and emotional dysregulation.
Key factors that contribute to substance use during seasonal transitions include:
- Dramatic changes in daylight exposure
- Disrupted sleep and circadian rhythms
- Increased feelings of isolation and loneliness
- Reduced social interactions
- Physiological stress responses
Understanding these intricate connections is crucial for developing effective treatment strategies for addiction and mental health that address both the underlying emotional challenges and potential substance abuse patterns.
Risk Factors Unique to Los Angeles Area
National research indicates that Seasonal Affective Disorder (SAD) disproportionately impacts certain demographic groups, with unique characteristics particularly relevant to the Los Angeles metropolitan landscape. Women are statistically more vulnerable to developing seasonal depression, and young adults represent the most at-risk population for experiencing these cyclical mood disorders.
Los Angeles presents distinctive environmental and social characteristics that can exacerbate seasonal depression and substance abuse risks. The region’s complex urban landscape, characterized by high-stress professional environments, diverse cultural pressures, and significant economic disparities, creates a perfect storm for psychological vulnerability. Entertainment industry dynamics, rapid lifestyle changes, and intense social competition can trigger significant mental health challenges that intersect with seasonal mood fluctuations.
Climate variations in Southern California, while more subtle than in other regions, still produce meaningful psychological impacts. Unlike locations with dramatic seasonal shifts, Los Angeles experiences nuanced environmental changes that can subtly influence mood and behavioral patterns. The region’s consistent sunshine might paradoxically mask underlying depressive symptoms, making early detection and intervention more challenging for mental health professionals.
Key risk factors specific to the Los Angeles area include:
- High-stress professional environments
- Intense social and professional competition
- Rapid lifestyle and economic transitions
- Complex cultural expectations
- Potential social isolation despite urban density
Understanding these localized risk factors is crucial for developing targeted mental health and addiction recovery strategies that address the unique psychological landscape of urban Southern California.
Effective Treatment for Co-Occurring Conditions
Integrated treatment approaches are crucial when addressing the complex intersection of seasonal depression and substance abuse. Clinical research demonstrates that comprehensive treatment strategies typically involve a multifaceted approach, incorporating medical interventions, therapeutic techniques, and holistic wellness practices.
The most effective treatment protocols recognize the intricate relationship between mental health disorders and addiction. Therapeutic research highlights that targeted interventions can not only alleviate immediate symptoms but also provide preventative strategies for future depressive episodes. This approach might include combinations of:
- Specialized counseling techniques
- Targeted medication management
- Light therapy interventions
- Nutritional and lifestyle modifications
- Comprehensive psychological support
Mental health professionals recognize that addressing co-occurring conditions requires a nuanced, personalized approach. The treatment must simultaneously target the underlying seasonal depression while providing robust support for potential substance abuse challenges. Cognitive behavioral therapy, group counseling, and individualized treatment plans can help individuals develop sustainable coping mechanisms that extend beyond seasonal limitations.
Psychological resilience becomes a critical component of long-term recovery. Patients benefit from learning adaptive strategies that help them navigate emotional fluctuations, recognize potential triggers, and build robust support systems. Substance abuse and depression recovery strategies emphasize developing comprehensive skills that promote mental wellness and reduce the risk of relapse during challenging seasonal transitions.
Supporting Loved Ones During Seasonal Changes
National mental health research emphasizes the critical importance of recognizing and responding to seasonal depression symptoms in loved ones. Understanding the subtle signs of Seasonal Affective Disorder (SAD) can be the first crucial step in providing meaningful support and preventing potential mental health complications.
Compassionate intervention requires a delicate balance of empathy and proactive support. Clinical guidelines highlight the serious potential consequences of untreated seasonal depression, including social withdrawal, work performance challenges, and increased vulnerability to substance abuse. Family members and friends play a pivotal role in identifying early warning signs and encouraging professional support.
Effective support strategies involve creating a supportive environment that acknowledges the individual’s emotional experiences without judgment. This might include:
- Maintaining open and non-confrontational communication
- Encouraging professional mental health consultations
- Helping establish consistent daily routines
- Participating in shared activities that promote positive mood
- Offering practical assistance during challenging periods
Recognizing that each person’s experience with seasonal depression is unique is essential. Some individuals may resist help or feel ashamed of their struggles. Patience, consistent emotional support, and understanding addiction and depression dynamics can create a foundation of trust that helps loved ones feel supported and empowered to seek necessary treatment.
Find Hope and Healing from Seasonal Depression and Addiction Today
Seasonal depression can deepen the struggle of addiction by fueling urgent emotional pain and the urge to self-medicate. If you or a loved one notice signs like persistent mood changes during certain seasons or increased substance use as a coping mechanism you are not alone. This article highlights how Seasonal Affective Disorder creates unique challenges that require compassionate, integrated care targeting both mental health and addiction.
At Glendora Recovery Center we specialize in treating co-occurring disorders with customized approaches including therapy, medical support, and flexible scheduling that fits your life. Do not wait until seasonal cycles worsen your symptoms reach out now for a confidential consultation. Discover how our expert team in Los Angeles County can guide you toward lasting recovery with our Partial Hospitalization Programs and Intensive Outpatient Programs. Take your first step to better days by contacting us at Glendora Recovery Center today.
Frequently Asked Questions
What is Seasonal Affective Disorder (SAD)?
Seasonal Affective Disorder (SAD) is a type of depression that occurs at certain times of the year, typically during fall and winter months, characterized by recurring mood episodes that significantly disrupt daily functioning.
How does Seasonal Depression influence substance abuse?
Individuals experiencing Seasonal Depression may turn to substances like alcohol or drugs as a coping mechanism, leading to a dangerous cycle of self-medication that can exacerbate both mental health and addiction issues.
What are the symptoms of Seasonal Depression?
Common symptoms of Seasonal Depression include persistent low mood, changes in energy levels and motivation, disrupted sleep patterns, social withdrawal, and increased vulnerability to substance abuse.
How can I support a loved one struggling with Seasonal Depression and addiction?
Support can include maintaining open communication, encouraging professional help, helping establish daily routines, engaging in uplifting shared activities, and offering practical assistance during tough times.
Recommended
- The Impact of Seasonal Shifts on Addiction Recovery Centers
- Depression in Recovery – How It Impacts Healing | Glendora Recovery Center
- Substance Abuse and Depression: Complete Guide | Glendora Recovery Center
- Bipolar Disorder and Addiction: Complete Guide | Glendora Recovery Center
- Coping With Seasonal Depression: Practical Tips That Work – Dr. Stephen Oreski & Associates